Retinal Vein Occlusion
A Retinal Vein Occlusion can occur when the circulation of a retinal vein becomes blocked and causes elevated pressure, which damages the vein, leading to hemorrhages, fluid leakages, swelling and a lack of oxygen in the Retina. This blockage can occur in the Central Retinal Vein or a Branch Retinal Vein. This can occur equally in women and men and mostly after the age of 60, and especially in those patients with diabetes, hypertension or cardiovascular disease. The visual symptoms of Retinal Vein Occlusion can vary greatly in severity from one person to the next and whether the Central Retinal Vein or Branch Retinal Vein has become blocked. Typically, patients experience a sudden onset of blurry vision or a “missing area of vision” if a branch retinal vein is occluded. A severe loss of central vision is more common if the central retinal vein has become occluded. Some patients who have Retinal Vein Occlusion will also experience a type of glaucoma as a secondary complication.
Patients who experience a Branch Retinal Vein Occlusion often notice a gradual improvement in their vision as the hemorrhage resolves. Unfortunately, visual recovery from a Central Retinal Vein Occlusion is much less likely since it is more likely to cause retinal ischemia (a severe lack of nutrition) leading to cell death.
Diagnosis of Retinal Vein Occlusion
To diagnose a Retinal Vein Occlusion your pupil will be dilated so that Center for Sight Retinal Specialist Robert Kelly, M.D. can directly observe the retina using special instruments including the ophthalmoscope and slit lamp with a high magnification lens so that fine detail can be examined. It is usually necessary to have an Intravenous Fluorescein Angiogram (IVF) to study the blood circulation in the retina, as well as an Ocular Coherence Tomogram (OCT) to detect the presence and severity of Macular Edema, or swelling.
Treatment of Retinal Vein Occlusion
The main objectives of treating Retinal Vein Occlusion are to avoid and treat secondary complications. If there are areas of the retina that have been deprived of oxygen there is the risk of growth of “new blood vessels” or “neovascularization” which are extremely fragile and easily broken, resulting in hemorrhage and scarring of the retina with resulting vision loss. The new blood vessels may also cause a type of secondary glaucoma, called Neovascular Glaucoma. If you develop neovascularization, it will be necessary to use Laser Photocoagulation Treatment and Vascular Endothelial Growth (VEGF) Inhibitor Injections to stop the growth of these delicate blood vessels.
Retinal Artery Occlusion
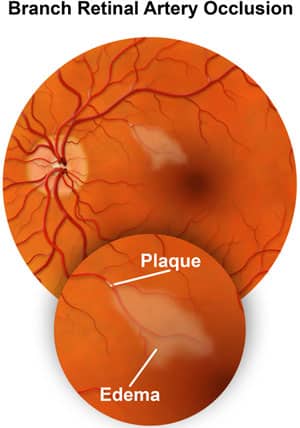
A Retinal Artery Occlusion can occur in either the Central Retinal Artery or in a Branch Retinal Artery. Either artery can become blocked by an “embolus” in the bloodstream. A Retinal Artery Occlusion is considered a stroke and requires immediate attention. When an artery occlusion occurs, it decreases the oxygen supply to the area of the retina nourished by the affected artery, causing permanent vision loss. Most patients who suffer Retinal Artery Occlusions are between the ages of 50 and 80. They notice a sudden, painless loss of vision that can be a complete loss of vision if it is a Central Retinal Artery Occlusion, or can be a partial loss of their visual field if it is a Branch Retinal Artery Occlusion. Sometimes the major loss of vision is preceded by one or more episodes of a “Amaurosis Fugax” or Transient Ischemic Attack (TIA).
Often, patients who have Retinal Artery Occlusions have other significant health problems such as high blood pressure, diabetes, heart arrhythmias or high cholesterol. Another possible cause of Retinal Artery Occlusion in patients over the age of 60 is an underlying inflammatory condition called Giant Cell Arteritis. Some patients who have Retinal Artery Occlusion will also experience a type of glaucoma as a secondary complication.
In the event that Center for Sight Retinal Specialist Robert Kelly, M.D. diagnoses you with a Retinal Artery Occlusion, or identifies a warning sign that you might be at risk for a Retinal Artery Occlusion because he observes the presence of a “plaque” in one or more of your retinal arteries, he will promptly refer you to your Internist or Cardiologist for thorough evaluation and testing including a blood pressure evaluation, electrocardiogram (EKG), fasting blood glucose, lipid and cholesterol levels, and hyper viscosity studies in order to help better understand your overall health.
Treatment of Retinal Artery Occlusions
Central Retinal Artery Occlusion is a type of stroke—as such, if it is recent, then treatment in an Emergency Room might be appropriate. In the past, a number of methods have been tried to dilate or widen the artery so as to free the embolus. However, large scale studies have shown that the only effective treatment is thrombolysis as part of a stroke protocol. These protocols are only effective when used when the artery occlusion is very recent, typically less than 4 hours old.
If you have any type of systemic vascular disease and need to be evaluated for your risk of Retinal Vascular Disease such as Retinal Artery Occlusion or Retinal Vein Occlusion, please call us to schedule an appointment at Center for Sight in Fall River, Massachusetts at 508-730-2020.
Retinal Detachment Symptoms, Types & Treatment
Retinal Detachment is a serious medical problem that requires rapid emergency treatment to try to prevent severe vision loss and possibly blindness. In normal, healthy eyes, the risk of Retinal Detachment is about 5 per 100,000 per year with a greater frequency in the middle aged or elderly population of perhaps 20 per 100,000 per year. Retinal Detachment is more frequent if you are myopic or nearsighted and especially if your prescription is above 6.00 Diopters of correction. In fact, 67% of Retinal Detachment cases occur in myopic eyes. Further, Retinal Detachment is more prone to occur in association with certain eye conditions and diseases including after cataract surgery and in patients suffering from Diabetic Retinopathy. Fortunately, with modern cataract surgery and early treatment of Diabetic Retinopathy, the incidence of Retinal Detachment is low.
Symptoms of Retinal Detachment
Symptoms you may experience if you have a Retinal Detachment include flashes of light that may occur in your field of vision toward the outermost periphery, a sudden increase in floaters in your vision and possibly even a ring of floaters or “hairs” in your vision, and/or a sense of a “shadow”, “curtain” or a “veil” being drawn over your in your peripheral vision, and in extreme cases you may experience a loss of central vision.
Types of Retinal Detachment
Rhegmatogenous Retinal Detachment
Rhegmatogenous Retinal Detachment occurs as a result of a break—usually a tear or hole—in the retina that permits fluid to pass into the space underneath the Retina. Rhegmatogenous Retinal Detachment is the most common type of Retinal Detachment.
Exudative Retinal Detachment
Exudative Retinal Detachment can occur due to inflammation, injury or a Retinal Vascular Disease that causes fluid accumulation underneath the Retina without the presence of a Retinal Hole or Retinal Tear.
Tractional Retinal Detachment
Tractional Retinal Detachment can occur when fibrous or fibrovascular scar tissue has been formed on the Retina as a result of an injury, inflammatory disease or the presence of neovascularization, such as in Diabetic Retinopathy. The scar tissue actually pulls the Retina free from the underlying pigment layer it is normally attached to, causing a Retinal Detachment.
Treatment of Retinal Detachment
Treatment for Retinal Detachment will depend on the cause, type and severity but can include:
Cryopexy and Laser Photocoagulation Treatment
Cryopexy and Laser Photocoagulation Treatment create a scar around the edge of a Retinal Hole, or small Retinal Tear in order to prevent fluid from passing through the hole and accumulating underneath the Retina. Cryopexy uses a cold instrument, about the size of a pencil, to scar the damaged area whereas Laser Photocoagulation Treatment uses a laser beam to create the scar. Cryopexy, usually reserved for very anterior tears only, is performed in an operating room, while laser treatment can often be done in the office.
Pneumatic Retinopexy
Pneumatic Retinopexy is used to inject a “gas bubble” into the back of the eye. The patient’s head is positioned so that the “gas bubble” acts to place gentle pressure against the detached retina, slowly pushing it back into place. This may require that patients lie perfectly still in a particular position for several hours or up to several days. Laser or cryopexy, usually performed after the gas injection, is then applied around or over the retinal tear.
Scleral Buckle Surgery
Scleral Buckle Surgery is performed by carefully sewing silicone bands to the outside of the eye in order to apply gentle pressure to the outermost walls of the eye so they move up against the Retinal Breaks, allowing the defect to close and the Retina to reattach. Scleral Buckle Surgery may be done in conjunction with Cryopexy or Laser Photocoagulation to assure the best possible results.
Vitrectomy
Vitrectomy is an increasingly common treatment for Retinal Detachment that involves surgically removing the Vitreous gel in the back part of the eye in conjunction with the injection of a “gas bubble.” In general, Vitrectomy is not the first surgery that is used to repair a Retinal Detachment because it often leads to the formation of a Cataract and should the initial surgery fail to allow reattachment of the Retina, the second procedure is often much more difficult and complex.
After surgery for Retinal Detachment, the results can often take many weeks for patients to achieve their visual recovery. In certain cases, the vision after Retinal Detachment Surgery may not allow the full recovery of precise vision, especially if the Macula was detached. Early diagnosis and rapid treatment are the keys to preventing vision loss from Retinal Detachment. Regular eye examinations are an excellent way to learn if you are at risk for Retinal Detachment.
If you experience the sensation of a curtain or a veil in your vision or if your vision becomes “bent” or distorted perhaps with the sensation of a “bubble”, you need to be evaluated immediately for Retinal Detachment. Please call us, explain your symptoms, and schedule an URGENT appointment at Center for Sight in Fall River, Massachusetts at 508-730-2020. Please relay your symptoms to the receptionist so that we can examine you IMMEDIATELY!

