Many patients are under the impression that glaucoma is just due to a high pressure within the eye. While a high intraocular pressure (IOP) certainly can be one cause of glaucoma, and in fact is the most common cause, a high IOP is not the only cause of glaucoma. It is entirely possible to have a higher than normal Intraocular Pressure (IOP) and vision loss and simply not know it. Fortunately, glaucoma is treatable, and in many cases patients retain excellent vision throughout their lives.
How Often Should I Be Checked for Glaucoma?
At Center for Sight, we recommend that all patients over 50 years of age who have no previous family history of Glaucoma or other general health conditions such as diabetes or high blood pressure, be evaluated for Glaucoma every two years. If there is any family history of Glaucoma at all, or there any other general health problems, we recommend patients be evaluated for Glaucoma every year beginning at age 40.
In addition, we now also know that there is considerable risk for siblings of those who have Glaucoma. In the Nottingham Glaucoma Study, it was found that the siblings of Glaucoma patients are 5 times the risk for developing Glaucoma by the age of 70 and therefore should be examined every year.
Glaucoma Risk Factors
Everyone is at risk for Glaucoma, however there are many factors that can predispose you to developing Glaucoma including:
Types of Glaucoma
Primary Open Angle Glaucoma
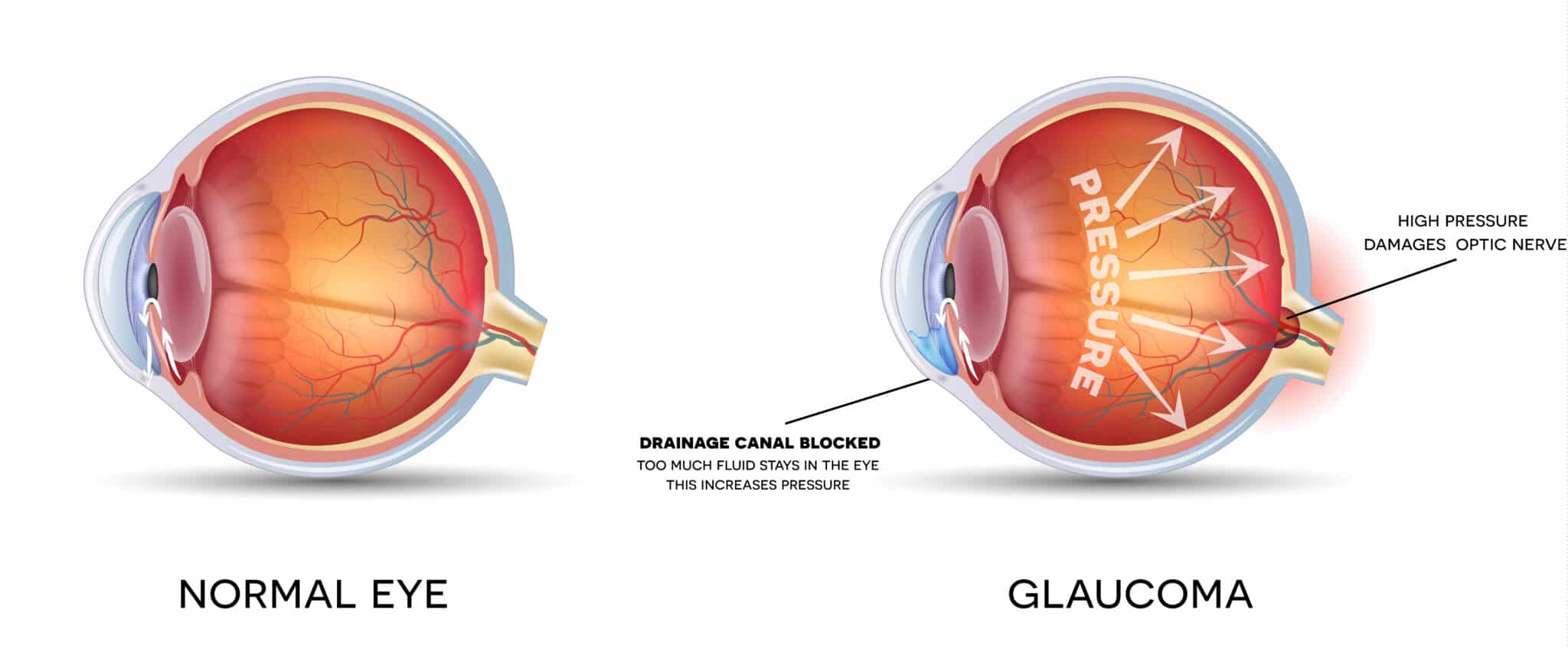
Primary Open Angle Glaucoma (POAG) is the most common type we see. Patients with Primary Open Angle Glaucoma usually have an increase in Intraocular Pressure (IOP) from either too much Aqueous Humor being produced or too little being drained from the eye. The fluid buildup within the closed space of the inside of the eye causes the pressure to rise. This elevation in pressure (IOP) causes the circulation in the optic nerve to decrease, depriving it of oxygen and nutrients, resulting in permanent damage to the optic nerve resulting in vision loss. If left untreated, an elevated Intraocular Pressure (IOP) may, over time, cause total blindness.
Angle Closure Glaucoma
There are two types of Angle Closure Glaucoma: Primary Angle Closure Glaucoma and Acute Angle Closure Glaucoma. Although Angle Closure Glaucoma occurs much less frequently than Open Angle Glaucoma, it is important because it can result in considerable vision loss in a brief period of time. Primary Angle Closure Glaucoma accounts for approximately 10% of all cases of glaucoma and about 2/3 of these once again produce no early symptoms for patients. Acute Angle Closure Glaucoma is one of the only types of glaucoma that produce distinct symptoms that include pain, light sensitivity, redness, blurred vision, colored haloes around lights and nausea or vomiting.
There are several causes of Angle Closure Glaucoma, but it is most often caused by anatomical changes within the internal structures of the eye. Angle Closure Glaucoma is considerably more common in farsighted eyes, which tend to be smaller and in patients between the ages of 45-60 years of age where the Crystalline Lens is beginning to swell.
During your general eye exam if the Center for Sight eye doctor observes or measures a narrowed angle, he or she will perform an additional examination procedure called Gonioscopy. If you are at risk for Angle Closure Glaucoma or have Acute Angle Closure Glaucoma your eye doctor may initially prescribe some medication to begin to lower the pressure and then will most likely recommend performing a “Laser Iridotomy,” which is quite successful in treating Angle Closure Glaucoma and preventing recurrences. Laser Iridotomy is a type of Laser Eye Surgery that the eye physicians and surgeons at Center for Sight will perform right in the comfort and convenience of our office.
Glaucoma is a very complex eye disease, and not simply an elevated Intraocular Pressure (IOP). Nonetheless, when detected early it can be successfully treated. Center for Sight and its staff provide the full scope of advanced technology diagnostic testing and treatment, as well as taking the time necessary to give each patient the personal education needed to fully understand their condition and get the best possible outcomes for their patients.
Glaucoma Diagnosis, Tests & Treatment
Diagnosing Glaucoma
Several diagnostic tests may be performed to make the most precise diagnosis of glaucoma. These include the following:
Tonometry
The Tonometry Test is a method of measuring your Intraocular Pressure (IOP). This test involves first placing some eye drops into your eyes to numb them and then lightly touching the surface of the cornea with a specialized measuring instrument.
Fundus Lens & Ophthalmoscopy
Fundus Lens & Ophthalmoscopy are methods of carefully examining the inside of the eye-especially the optic nerve. Dilating eye drops will be placed in your eyes so that clear and direct observation of the optic nerve is possible.
Additional Glaucoma Testing
If either your Intraocular Pressure (IOP) is elevated or your optic nerve appears unusual, additional tests will be necessary to complete the glaucoma examination. These may include the following test procedures:
Optic Nerve Stereo Photography
A special camera may be used to obtain stereoscopic photographs of your optic nerves. These provide a useful objective record of your optic nerve appearance against which future comparisons may be made.
Visual Field Perimetry
Perimetry or Visual Field testing is an important part of the glaucoma examination where you will be asked to sit in front of a large “bowl like” instrument and a computer program will present a small lights in different positions of your “side” or peripheral vision to see how far your side vision extends in various directions. The computer will then plot an actual map of your field of vision.
Gonioscopy
By using a special contact lens, gonioscopy is a quick and painless test that allows us to directly observe the health and condition of the angle where the iris meets the cornea and evaluate your risk for the angle to become closed.
Optic Nerve Computer Imaging
Using OCT or Optical Coherence Tomography we capture digital images with special beams of light in order to create a contour map of the optic nerve and measure the retinal nerve fiber thickness.
Pachymetry Measurement of Corneal Thickness
Corneal thickness is important because it can alter the accuracy of the measurement of Intraocular Pressure, potentially causing doctors to delay necessary treatment in some cases or causing doctors to treat normal people unnecessarily in other cases. Your actual Intraocular Pressure may be UNDERESTIMATED if you have thin corneas and it may be OVERESTIMATED if you have thicker corneas.
Glaucoma Treatment
There are three main methods of treating glaucoma: Medical, Laser and Surgical. These treatment options for controlling glaucoma are quite important, as glaucoma has no cure. In almost all cases, glaucoma is treatable, but must be diagnosed as early as possible. The following information is limited to treatment of Primary Open Angle Glaucoma, as it is the most common type of Glaucoma. Primary Open Angle Glaucoma is treated by the three different approaches above depending on the severity of the disease and the ability of each treatment option to slow or halt the disease progression and preserve your vision.
Medical Treatment of Glaucoma
Primary Open Angle Glaucoma is most often treated by prescribing one or more types of eye drops to lower your Intraocular Pressure (IOP). By using a single type of medication or sometimes 2 eye drops in combination, more than 80% of the patients with Open Angle Glaucoma can be successfully treated. These eye drops work by either decreasing the amount of fluid being produced inside your eye or by increasing the rate of drainage of fluid from your eye. For most patients, using the eye drops as prescribed-1-2 times per day it is possible to control the Intraocular Pressure (IOP) and slow or even halt the loss of vision.
Laser Treatment of Glaucoma
The use of laser treatment for glaucoma has become an important treatment option for many patients. In the past, laser treatment for glaucoma was considered a “last resort” before glaucoma surgery. Today, thanks to advances in lasers, using a laser treatment for glaucoma in conjunction with the eye drop treatment or sometimes even using the laser treatment as the primary treatment are excellent options to help maintain control and slow or stop the progression of the disease.
Surgical Treatment of Glaucoma
For a small number of patients, even with the maximum medical therapy and laser treatment, it is still not possible to achieve good stable control of their disease and stop the progression of vision loss. For these patients, there are surgical procedures available to help achieve control of the Intraocular Pressure (IOP) and slow or stop the progression of the disease that include removing a tiny piece of the Trabecular Meshwork, a surgical procedure called “Trabeculectomy”, “Sclerostomy” or “Filtering Procedure”, or even implanting microscopic glaucoma valves, stents such as the iStent®, shunts such as the Ex-PRESS Mini Shunt and tubes to help reduce and stabilize the Intraocular Pressure (IOP) and prevent vision loss.
If you or a family member or friend have not had a recent glaucoma screening or glaucoma exam and would like to have the diagnosis of glaucoma ruled out with the appropriate glaucoma tests or glaucoma treatment if necessary, please make an appointment by at Center for Sight in Fall River, Massachusetts at 508-730-2020.



