Herpes Zoster Keratitis (Shingles)
Herpes Zoster Keratitis is caused by the same virus that causes chicken pox and shingles, called Varicella-Zoster Virus. It is possible that after having chicken pox as a child, the Varicella-Zoster Virus remains in the nerve cells in an inactive state. The Varicella-Zoster Virus can reactivate later in life and travel through the nerves in different parts of the body causing a painful blistering rash. If the Varicella-Zoster Virus travels to the head, it can affect the eye and thus cause a corneal infection.
Ocular Herpes and Herpes Keratitis
Ocular Herpes, or Herpes of the eye is caused by the Herpes Simplex Virus and is a common causes of corneal blindness in the United States. People who have a single Herpes Simplex viral infection of the eye can experience a flare up or recurrence. The virus often leads to irreversible scarring of the cornea. Ocular Herpes may start as a painful sore on the eyelid or surface of the eye. If left untreated, it may multiply and begin to destroy epithelial cells and progress deeper into the cornea. If the Ocular Herpes penetrates the deeper layers of the cornea, it may cause corneal scarring. Prompt diagnosis and treatment of Ocular Herpes is important.
Fuchs’ Dystrophy
Fuchs’ Dystrophy is a slowly progressive disease of the cornea that occurs when the innermost layer of cells, called the endothelium, prematurely weakens, making it less efficient in its “pumping activity” which is required to maintain transparency for clear vision. Sometimes Fuchs’ Dystrophy can occur in people in their 30’s and 40’s, but most often does not compromise vision until people are in their 50’s or 60’s. Early in the course of Fuchs’ Dystrophy, there may be blurry vision in the morning that gets progressively clearer as the day passes. In its later phases, Fuchs’ Dystrophy is often associated with considerable pain as the epithelium blisters called “bullae.” Many patients with Fuchs’ Dystrophy that require surgery to restore vision may benefit from a technique called Descemet’s Stripping with Endothelial Keratoplasty (DSEK). This type of corneal transplant involves only the diseased portion of the cornea.
Map-Dot-Fingerprint Dystrophy
The outermost layer of the cornea, called the epithelium, is attached to an underlying basement membrane called Bowman’s Membrane. Sometimes the epithelial basement membrane develops abnormally making it difficult or impossible for the epithelium to adhere properly to the basement membrane. If the epithelium does not adhere properly, Recurrent Corneal Erosions can occur. Recurrent Corneal Erosions are painful and cause the corneal surface to become irregular, resulting in intermittent blurry vision along with the discomfort and foreign body sensation. Map-Dot-Fingerprint Dystrophy is also known as Epithelial Basement Membrane Dystrophy because it is caused by a lack of the healthy formation of the Basement Membrane. It affects adults between the ages of 40-70 and can sometimes begin earlier. As the name implies, its appearance is of a map of gray areas accompanied by opaque dots and fingerprint-like whirls or lines. The best treatment results can be achieved using superficial lamellar Keratectomy or amniotic membrane placement.
Lattice Dystrophy
Lattice Dystrophy occurs from the accumulation of abnormal protein fibers, or amyloid deposits in the middle cornea layer called the corneal stroma. If these deposits become dense enough they will become opaque and affect the corneal transparency so that vision is reduced. If these deposits occur under the outermost layer, the epithelium, they can cause recurrent erosions of the cornea, which can be painful and disturb the normal corneal curvature, effecting vision. In instances where there are recurrent corneal erosions and pain, the doctor may prescribe eye drops, ointments and occasionally an eye patch or bandage soft contact lens. Early Lattice Dystrophy seems to respond well to Excimer Laser Phototherapeutic Keratectomy (PTK) whereas more serious cases may require a corneal transplant.
Pterygium
A pterygium is a fleshy triangular growth of tissue on the cornea that may grow slowly throughout a person’s life. People who live in sunny climates where they are exposed to more sunlight and wind are more prone to developing pterygia. Pterygia can grow across the cornea and block the pupil. Pterygia may become red, swollen and inflamed. Under certain circumstances, they may need to be removed. Dr. Johnson performs pterygium excision using a conjunctival graft to prevent recurrences and obtain the best possible results after pterygium surgery.
Corneal Transplants
A corneal transplant is a type of corneal eye surgery performed in order to replace diseased, damaged or scarred corneal tissue with new healthy corneal tissue. Since damaged or scarred corneal tissue does not allow light to effectively pass into the eye and reach the retina, poor vision and even blindness may result from a damaged cornea. There are various types of corneal transplants Dr. Johnson may use to replace unhealthy corneal tissue.
Penetrating Keratoplasty
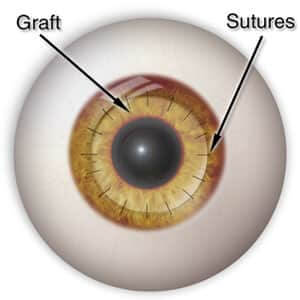
Penetrating Keratoplasty involves the surgical removal of the central, full thickness of the damaged cornea, and replacement with a clear cornea obtained from the eye bank. The donor cornea is secured with sutures that are thinner than a human hair. To facilitate the healing of the new transplanted cornea, Dr. Johnson prescribes eye drops for patients who have had corneal transplants. After she has determined that the new cornea has healed properly, Dr. Johnson will remove the fine sutures. The use of a contact lens might be required for the clearest vision after surgery.
Superficial Lamellar Keratoplasty
Superficial Lamellar Keratoplasty may be performed if the damaged corneal tissue is located in the cornea. Essentially, Dr. Johnson will carefully dissect the outermost layer of the cornea and remove it along with the damaged tissue. New, healthy tissue then heals on the cornea.
Descemet’s Stripping with Endothelial Keratoplasty (DSEK)
Descemet’s Stripping with Endothelial Keratoplasty (DSEK) is performed through a small incision to remove and replace the inner cell layer of the cornea when it stops working properly. With this technique, the surgeon gently strips off the single diseased cell layer, called the endothelium, and leaves the remaining cornea intact. Dr. Johnson replaces this layer with donor tissue from the eye bank. She will then insert an air bubble to unfold and position the donor tissue on the recipient cornea. Within a few minutes the donor tissue attaches to the recipient. There are several advantages of DSEK, including the eye remaining much stronger, a quicker visual recovery and minimal change in your eyeglass prescription.
Corneal Specialist
At Center for Sight, Keegan S. Johnson, M.D. is fellowship trained Corneal Specialist who provides exams, consultation and treatment for the full range of medical and surgical conditions affecting the cornea including corneal infections, corneal dystrophies, keratoconus, trauma and pterygia. It is often possible to treat these conditions with eye drops or other medications, surgery or contact lenses.
If you or a family member or friend needs treatment for corneal diseases, infections, dystrophies or corneal transplant surgery, please take a moment to request an appointment by calling Center for Sight in Fall River, Massachusetts at 508-730-2020.

